Taking flight against malaria: How Rwanda and Zipline are changing the story
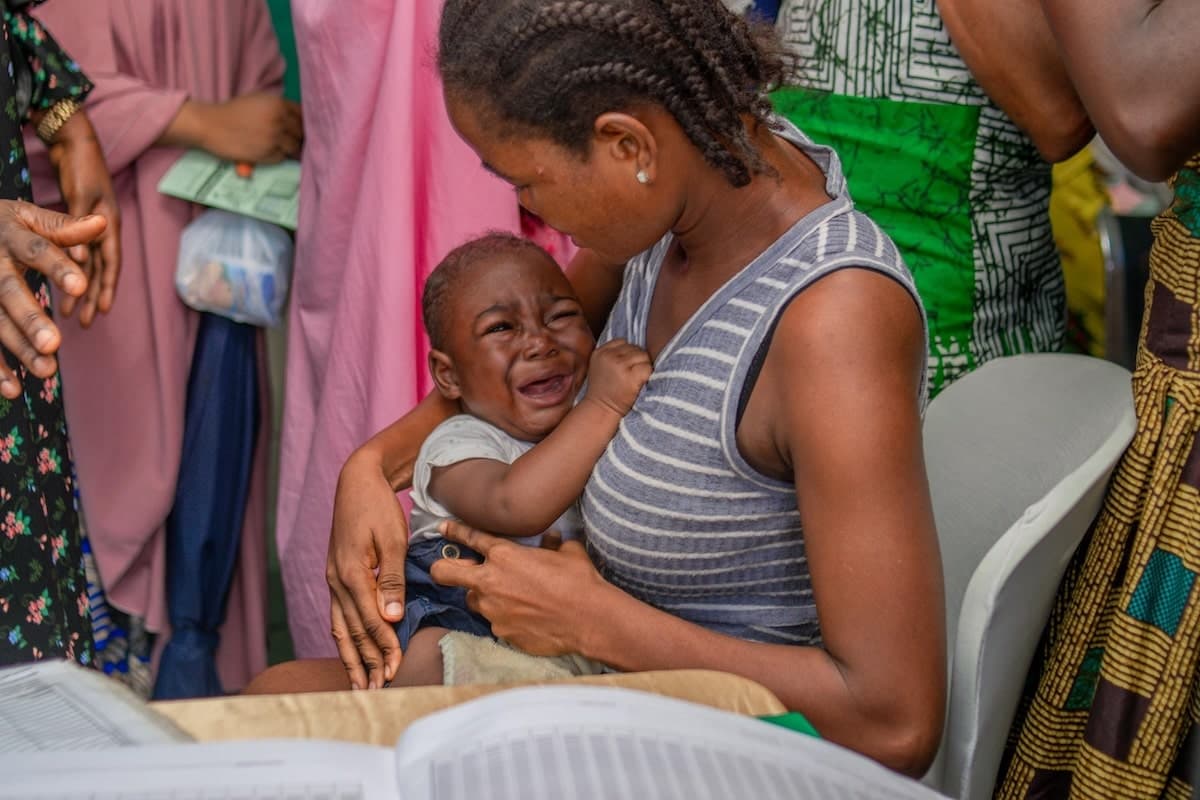
At a health facility in Nyagatare, a distraught mother anxiously holds her four-year-old child who is burning with fever. She has just been told the health facility has run out of malaria medication—again.
This heartbreaking scenario is all too familiar for families across Rwanda’s remote communities. Malaria remains a persistent threat, and although preventable and treatable, the disease has resurged. Severe cases have risen by 50 percent in Rwanda over the past year alone, reversing years of hard-won progress and placing thousands more lives at risk.
Delayed treatment, drug and insecticide resistance, and inconsistent access to essential medicines are driving this crisis. Sub-Saharan Africa’s warm, humid climates create ideal breeding conditions for malaria-carrying mosquitoes, making Rwanda especially vulnerable. With the influence of climate change, the situation could worsen over the coming decades.
Rwanda is responding with urgency and a novel approach. In a 12-month pilot led by the Rwanda Biomedical Centre (RBC) and Zipline, autonomous drones now deliver essential malaria treatments like Artesunate on demand to 70 health facilities across Nyagatare, Gisagara, and Nyamasheke. These districts were chosen for their high burden of severe malaria and difficult road access. Zipline’s rapid deliveries are helping reduce delays, prevent stockouts, and allow health workers to act before symptoms become life-threatening.
Speed, Trust, and Smarter Systems
In areas where malaria is endemic, timely access to medication is critical, especially for children under five. Before Zipline, many rural health facilities routinely faced shortages of second-line malaria treatments, forcing patients to wait hours or even days for resupply.
Health staff at Gakoma Hospital in Gisagara District have already noticed significant improvements since the start of this pilot. One staff member explained, "Previously, emergency requests took around two hours from the time an order was placed with the regional warehouse. Regular resupply orders could take up to one or even two days. Now, with Zipline, these medicines arrive in just 27 minutes."
Faster delivery means faster care and renewed community trust in the health system. Jackson Kalinijabo, Director of Health in Gisagara District, has seen firsthand the impact of Zipline’s service: "Receiving malaria commodities such as Artesunates via Zipline has been a game-changer for health facilities in Gisagara District. Faster drone deliveries translate directly to faster care, saving lives in our communities. We believe this innovative approach, alongside other interventions, brings us closer to eradicating malaria in our district."
But this shift isn’t just about speed. It’s about using Rwanda’s existing resources more effectively. With centralized inventory and on-demand delivery, health facilities no longer need to stockpile expensive second-line treatments like Artesunate-Pyronaridine or Dihydro-Artemisinin, which were, at times, indiscriminately used for non-severe cases. These medicines are now delivered only when needed, reducing waste and ensuring they are preserved for the most critical cases.
Centralization of malaria commodities for these districts with Zipline also minimizes expiration, lowers transport costs, and relieves pressure on rural clinics. Early treatment of malaria—before it becomes severe—not only improves patient outcomes but also eases the burden on the health system by reducing the high costs associated with treating advanced cases.
From Innovation to Eradication
This progress would not be possible without the visionary leadership of Rwanda’s Ministry of Health and the RBC. This marks the first time Zipline’s drone technology is being deployed specifically to support malaria response in the country. It also reflects Rwanda’s alignment with this year’s World Malaria Day theme: Reinvest, Reimagine, Reignite.
In a time of shrinking global health budgets, Rwanda is demonstrating how, with the application of proven technology, funding for health systems can be spent most efficiently.
The initiative is already reshaping care in remote areas. It’s expected to reduce severe malaria mortality by 40 percent and cut hospital referrals by 25 percent across the three districts. As the program advances, we are working closely with RBC to track results and explore how this model can scale to serve even more regions.